Plantar Fasciitis is the common term for what should be more accurately termed Plantar Fasciosis. itits is an acute inflammation caused by a trauma or infection. osis is chronic degenerative condition.
No evidence exists for an ideal treatment of this condition without identifying and treating the causes, which can be many. Since we have no literature to guide us, this advice comes from seeing hundreds of runners and guiding them in self corrections.
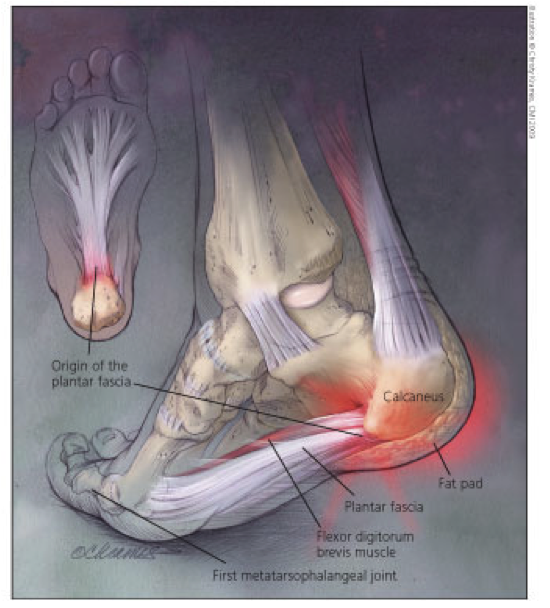
What is the Plantar Fascia?
The plantar fascia (PF) is a strong ligament that runs from the heel to the metatarsal heads in the front of your foot. This ligament helps absorb the shock that occurs when your foot contacts the ground. It has function in the windlass mechanism recreating the arch on takeoff.
What is the Cause of Plantar Fasciitis?
The PF is designed to manage a relatively small amount of stress. The intrinsic and extrinsic muscles of the foot are designed to receive signals from the fascia and in turn manage the majority of the load. When those muscles are dysfunctional the load gets transferred to the PF which is unable to handle it hence causing tears or plantar fasciitis. You can repair these tears by using palliative methods but as soon as you hit it again you will have to go through the same process. The only way that you can actually fix plantar fasciitis is to address the root cause... weak foot muscles. (Thank you Lance from Barefoot Science for the insight).
Several Structural Causes can Contribute to the Problem
- Weak intrinsic muscles of the foot
- A misaligned and weak first toe
- Tight shortened calf muscles
- Tight plantar fascia
Other Important Contributors
- Increased mechanical stress from the amount of running or activity
- Obesity
- Adapting too fast from supportive footwear which inhibits intrinsic muscles to flat shoes or barefoot (i.e. summer if going quickly into flip flops or barefoot)
- Poor walking and running mechanics
- Overly supportive footwear leading to instability. This is a paradox as shoes that over support will weaken the foot which in turn leads to the foot’s instability.
What Can You Do to Correct Plantar Fasciitis?
There are a few basic principles but they will vary depending on the cause:
- Any support from an orthotic, arch support, or taping should be a temporary modality while you strengthen and lengthen the tissues. Using one of these forever is akin to breaking your arm and leaving the cast on forever (in one week muscles begin to atrophy from disuse).
- Doing eccentric drop down exercises from a stair can help. Place your foot on stair and drop your heels down. It is OK to have a little pain doing this as long as it is getting progressively better.
- Dorsiflex the big toe to lengthen PF if it is tight
- Get out of heels - gradually - in ALL activities
- Work on foot intrinsics... pick things up with your foot. Walk barefoot.
- Practice a technique of running encouraging more natural form, ligher ground contact and loading rates, and more proprioceptive cueing. For more info, check out Chi Running by Danny Dreyer, Natural Running by Danny Abshire, Evolution Running by Ken Mierke, and the excellent teaching of Lee Saxby of Terra Plana VIVOBAREFOOT (see video).
- Strengthen your big toe by pushing it into the ground as often as you can whenever you are standing throughout the day. This will wake up the foot muscles and help recreate the arch.
- If you first toe is bent in consider a product to straighten it like Correct toes from Dr. Ray McClanahan.
- Use the principle of gradual progression and body sensing when making any changes
- Avoid NSAIDS (Motrin, Ibuprofen, etc). These drugs interfere with natural healthy healing processes.
- See a good health provider who understands natural running and walking

What About Orthotics?
Read this excerpt from Barefoot Science Canada (I am completely aligned with their opinion):
Source: http://www.barefoot-science.ca/plantarfasciitis.html
Custom orthotics and similar products attempt to stabilize the subtalar joint by supporting the arch, claiming to correct the poor biomechanics of the foot. This claim of correction is quite misleading. Orthotics only mask the symptoms by artificially supporting a dysfunctional structure along with its inherent muscle imbalances, while introducing a new angle of ground interface to the foot.
The artificial support provided by orthotics has little or no effect on the alignment or structural integrity of the interlocking bones that are still loose and unstable. The foot remains functionally unstable and will become increasingly weaker and dependent on the support. These bracing and supporting characteristics can actually prevent proper alignment in the foot and ankle as they manage multi-directional activities, contributing to increased stresses at the ankle and knee. And the chance of injury increases when misalignment and increased stress combines with an unlocked structure.
From a biomechanical perspective, by introducing a new angle of ground interface, orthotics cause a shift in the dynamics of the repetitive movement. The symptoms resulting from the old dynamic disappear and the problem seems to be corrected. Unfortunately, over time or with increased activity levels at the new ground interface angle, the repetitive movement often results in new symptoms at different locations. This creates a recurring cycle where new orthotics are prescribed to compensate for the ever-migrating symptoms and pathologies. The current practice is to recommend new orthotics at least every couple of years.
Heel-that-pain has some great exercises and videos including a nice demo on taping. The heel seat can also be a useful non supportive tool to give some short term relief while you strengthen the foot.
And finally do not wear shoes that shorten your PF or place your foot in all-day-dysfunction: wear minimalist footwear!
